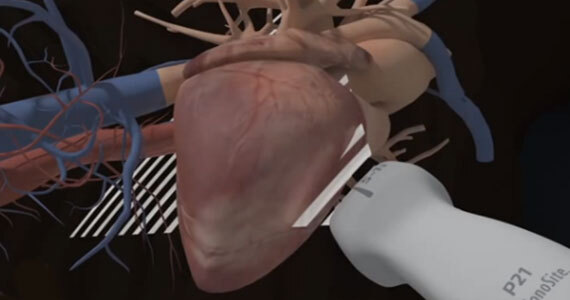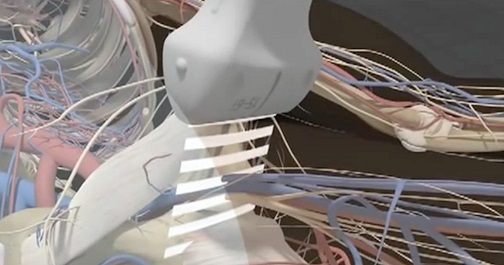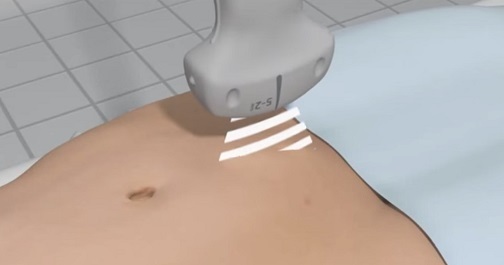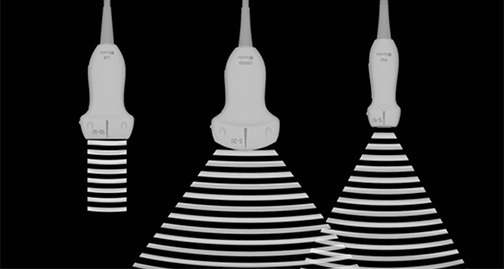
Aorta
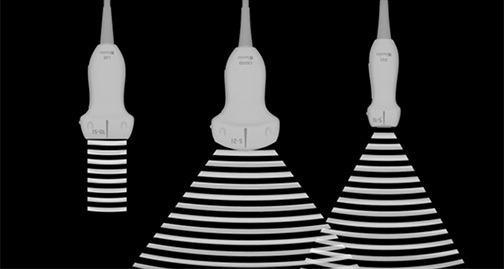
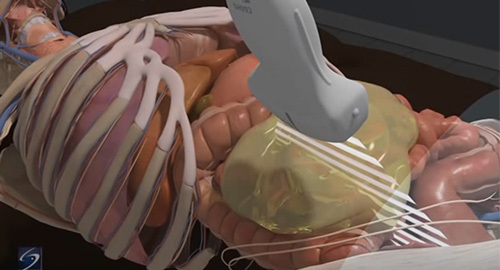
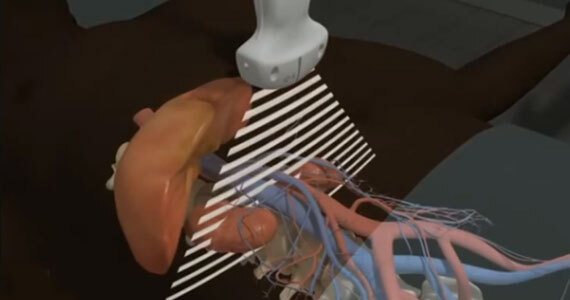
After completing the aorta ultrasound course, participants should be able to: identify the anatomical structures visualized during the aorta examination, recognize the various types of abdominal aortic aneurysms and perform their associated measurements, and determine the preferred transducer to perform the aorta exam.