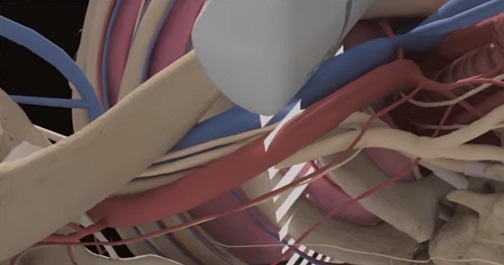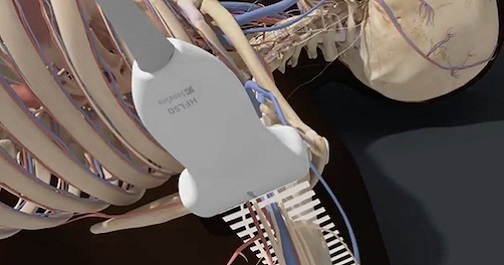
Axillary Nerve Block
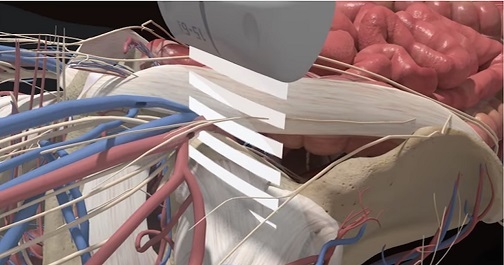
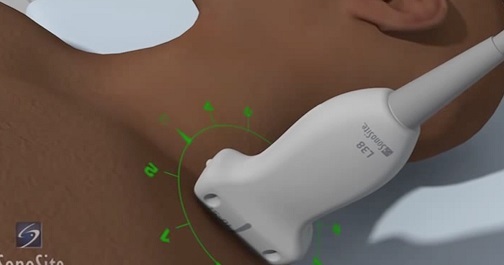
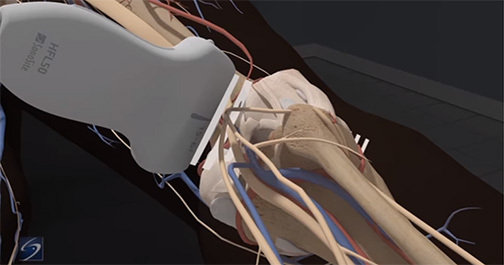
The axillary block is a plexus block at the terminal branches of the brachial plexus, designed to anesthetize the major motor and sensory nerves in the distal arm, elbow, wrist, forearm, hand, and fingers. Course participants will learn the anatomy of the axillary vessels and musculocutaneous nerve and the technique for performing an axillary nerve block.