*NEW* Resuscitative TEE - Transesophageal Ultrasound
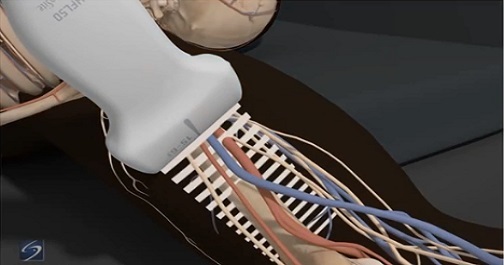
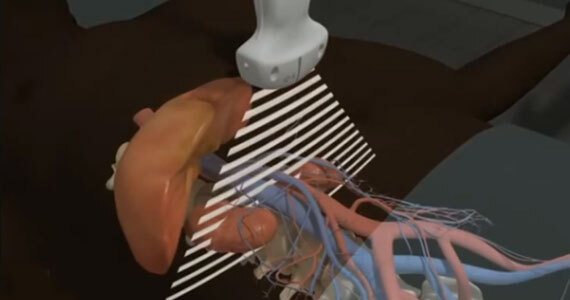
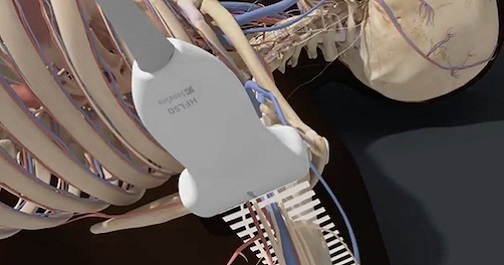
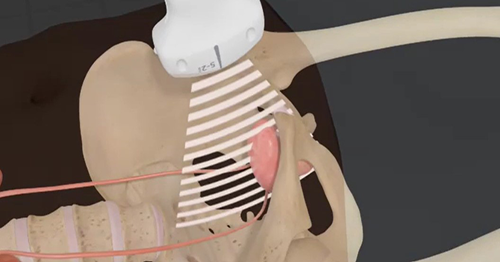
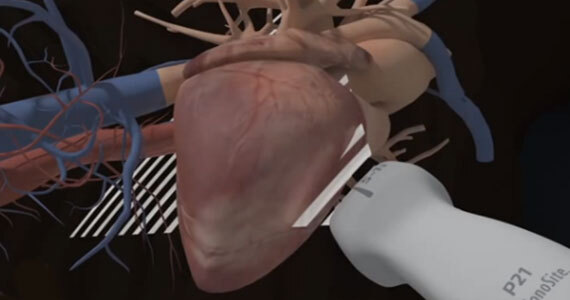
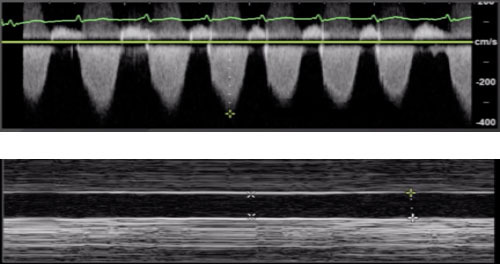
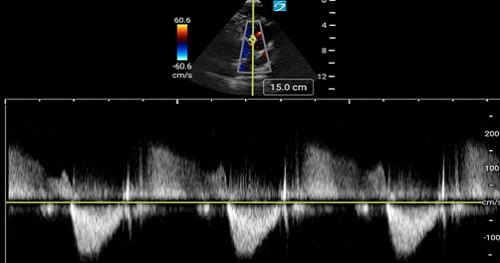
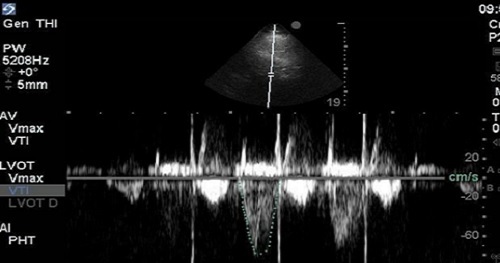
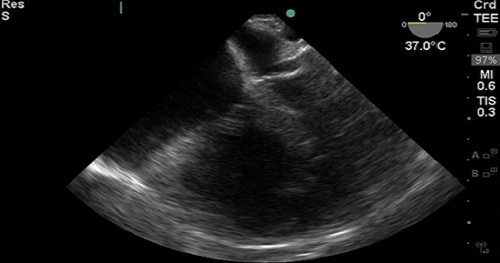
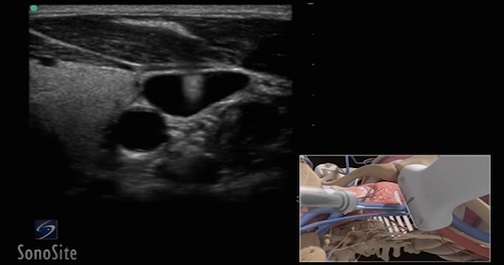
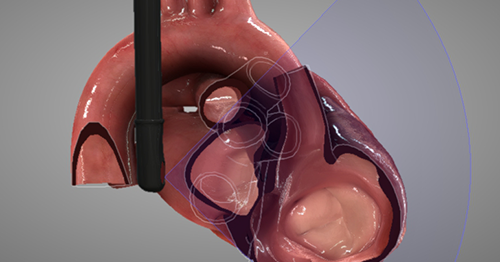
TEE at the point of care is an emerging modality that offers bedside clinicians the ability to assess critically ill patients quickly. A Transesophageal Echocardiogram, or TEE, is an alternative way to perform an echocardiogram. A specialized transducer containing an ultrasound transducer at its tip is passed into the patient's esophagus. This allows image and Doppler evaluation which can be recorded.